When you have asthma, using an inhaler with corticosteroids can change your life. For millions of people, it means fewer attacks, less wheezing, and the freedom to breathe without fear. But it’s not without trade-offs. While these medications are among the most effective tools we have for controlling asthma, they come with side effects that many patients don’t realize are preventable-or even reversible.
Let’s be clear: you should not stop your inhaler because you’re worried about side effects. Untreated asthma is far more dangerous. But you also shouldn’t just take it and hope for the best. The difference between safe use and risky use often comes down to three things: how you use it, how much you use, and how often you get checked.
What Are Inhaled Corticosteroids (ICS), Really?
ICS aren’t the same as the oral steroids athletes or bodybuilders use. These are designed to act right where they’re needed: in your airways. The medication is delivered as a fine mist or powder, so it lands directly on the inflamed lining of your lungs. This local action reduces swelling, mucus, and sensitivity-without flooding your whole body with hormones.
Common ICS brands include fluticasone, budesonide, mometasone, ciclesonide, and beclomethasone. Each works similarly, but they don’t behave the same way in your body. For example, ciclesonide has less than 3% systemic absorption, while fluticasone can absorb up to 40%. That’s why switching from one to another isn’t just a brand change-it can actually cut your risk of side effects in half.
The Two Types of Side Effects: Local vs. Systemic
Side effects fall into two buckets: local (happening right where the drug lands) and systemic (affecting your whole body).
Local side effects are the most common-and the most preventable. These include:
- Oral thrush (a yeast infection in the mouth)
- Hoarseness or voice changes
- Throat irritation or coughing after inhalation
According to a 2023 survey of over 1,800 asthma patients, 68% reported at least one of these. But here’s the good news: using a spacer and rinsing your mouth after each puff cuts thrush risk by more than half. Voice changes drop from over 30% to under 12% with consistent rinsing.
Systemic side effects are rarer but more serious. They happen when some of the drug gets into your bloodstream. The risk rises sharply with dose:
- Adrenal suppression (your body stops making its own cortisol)
- Bone thinning (especially over age 65 or after 5+ years of use)
- Increased risk of pneumonia (in older adults)
- Skin thinning and easy bruising
- Cataracts (in children on high doses)
A 2021 study found that patients taking fluticasone at 500 mcg/day or more had nearly three times the risk of adrenal suppression compared to those on budesonide at the same dose. And if you’re over 65 and on more than 500 mcg/day, your risk of pneumonia jumps from 5.2 to 8.9 events per 100 people each year.
Dose Matters More Than You Think
Many people think more inhaler puffs = better control. It’s the opposite. The goal isn’t to crush your asthma-it’s to keep it quiet with the smallest dose possible.
Experts agree: the relationship between dose and side effects isn’t linear. It’s a curve. Below 250 mcg of fluticasone equivalent per day, side effects are rare. Above 500 mcg, they start climbing fast. At 1,000 mcg/day, you’re entering the same risk zone as taking oral steroids.
Here’s what that means in real terms:
- Fluticasone: 100 mcg = low dose, 500 mcg = high dose
- Budesonide: 200 mcg = low dose, 800 mcg = high dose
- Ciclesonide: 160 mcg = low dose, 320 mcg = high dose
Many patients are on doses far higher than they need. A 2024 study found that 40% of people on ICS could have safely cut their dose by at least half without losing control. The key? Regular check-ins with your provider to test if you still need the same amount.
How to Use Your Inhaler Correctly (And Why It’s Life-Changing)
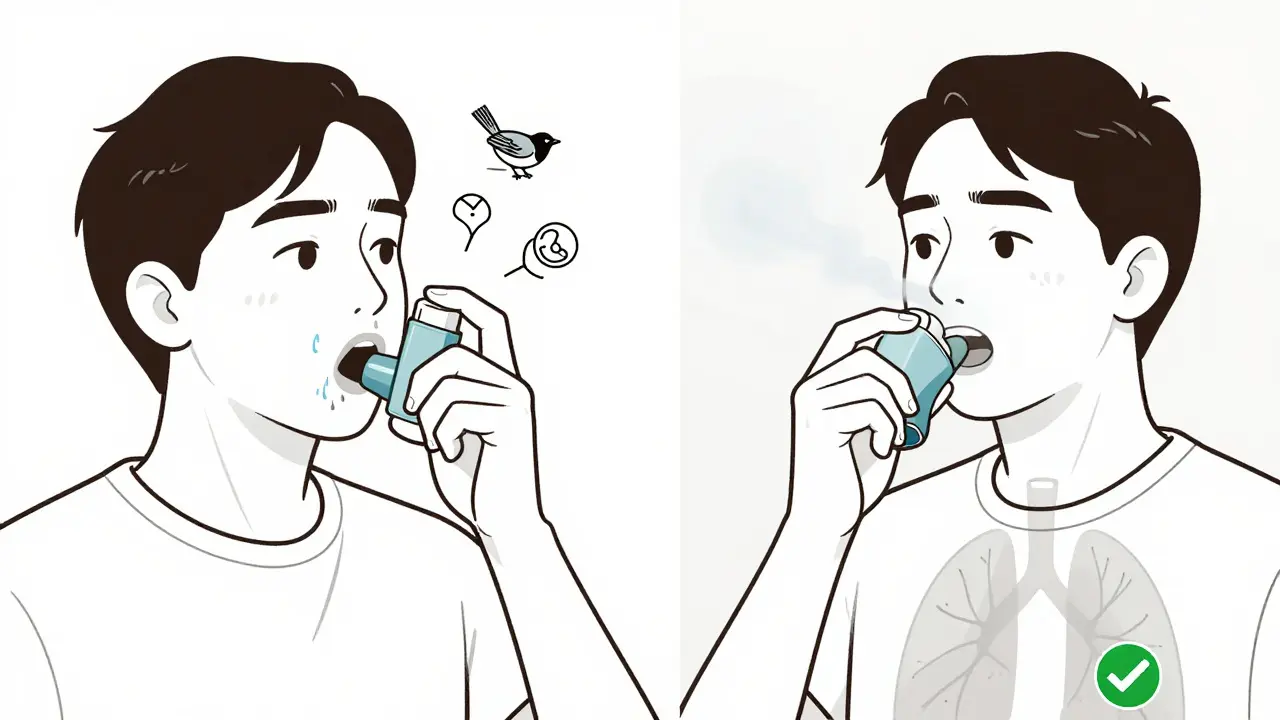
Most people use their inhalers wrong. Not because they’re careless-but because no one ever showed them how.
With a standard metered-dose inhaler (pMDI), only 10-20% of the medication actually reaches your lungs. The rest sticks in your mouth or throat. That’s why side effects happen.
Using a spacer changes everything. It holds the puff in a chamber so you can inhale slowly and deeply. Studies show it boosts lung delivery to 60-80% and cuts throat deposition by 70-80%. It’s cheap, reusable, and works with almost every inhaler.
And always rinse your mouth with water after each use. Don’t swallow it-just swish and spit. It’s that simple. Patients who do this regularly cut their risk of thrush from 38% to 14%.
Here’s the checklist no one gives you:
- Shake the inhaler well.
- Attach it to a spacer.
- Breathe out fully.
- Press the inhaler once, then inhale slowly for 5 seconds.
- Hold your breath for 10 seconds.
- Rinse your mouth with water and spit.
Do this every time. Even if you’re not sure you got it right. Your lungs will thank you.
Who Needs Extra Monitoring?
Not everyone needs the same level of oversight. But some groups are at higher risk and should be checked more often:
- Children under 12: High doses (over 800 mcg/day) may slightly slow growth, but studies show no long-term effect on adult height if doses are kept low. Still, annual height checks are recommended.
- People over 65: Watch for bone thinning and pneumonia. Ask for a bone density scan if you’ve been on high-dose ICS for more than 5 years.
- Pregnant people: Budesonide is the safest choice. Avoid fluticasone if possible-there’s less safety data.
- Anyone on more than 500 mcg/day: If you’re tired, bruise easily, or feel like you’re losing muscle tone, get your cortisol levels checked. A simple saliva test can catch adrenal issues before they become serious.
What’s New in Monitoring?
Technology is helping. Smart inhaler attachments now track when you use your device and whether your technique is correct. One device tested in 2023 caught technique errors in 92% of cases where people thought they were using it right.
Doctors are also starting to use blood tests. If your eosinophil count (a type of white blood cell) is above 300 cells/μL, you may be able to cut your ICS dose by half and still stay in control. This personalized approach is becoming standard in specialist clinics.
And new drugs are coming. AstraZeneca’s AZD7594, currently in trials, reduces adrenal suppression by 90% compared to fluticasone. In the future, biologics like dupilumab may replace ICS for many people with severe asthma-cutting steroid use by 70%.
The Bottom Line: You’re in Control
ICS are not dangerous if used correctly. They’re essential. But they’re not harmless, either. The side effects aren’t random-they’re predictable. And they’re preventable.
If you’ve been on an ICS for more than six months, ask yourself:
- Do I use a spacer?
- Do I rinse and spit after every puff?
- Do I know my exact daily dose in mcg?
- Has my dose been reviewed in the last year?
- Am I having any mouth, skin, or energy issues?
If you answered "no" to any of these, it’s time to talk to your doctor. You don’t need to live with hoarse voice or bruised skin. You don’t need to fear adrenal problems. You just need to know how to use your inhaler-and how to ask the right questions.
Low-dose ICS with good technique is one of the safest treatments in all of medicine. But high-dose ICS with bad technique? That’s where the real risk lies. Don’t assume your doctor is monitoring you. Take charge. Your lungs-and your whole body-depend on it.
Can I stop using my steroid inhaler if I feel fine?
No. Even if you feel fine, your airways may still be inflamed. Stopping suddenly can trigger a severe flare-up. Always work with your doctor to taper down slowly if you’re ready to reduce your dose. Never stop without medical guidance.
Is there a steroid inhaler with fewer side effects?
Yes. Ciclesonide and mometasone have much lower systemic absorption than fluticasone or beclomethasone. Budesonide is also safer than fluticasone at equivalent doses. Talk to your doctor about switching if you’re on a high-dose older inhaler and experiencing side effects.
How often should I get my inhaler technique checked?
At least once a year-but every 3 to 6 months is better, especially if you’ve had recent flare-ups or changes in your dose. Many patients make mistakes without realizing it. A quick demo from a nurse or pharmacist can save you from side effects and wasted medication.
Do I need a bone density scan if I’m on ICS?
If you’re over 65 and have been on more than 750 mcg/day of fluticasone (or equivalent) for over 5 years, yes. If you’re younger but have other risk factors for osteoporosis (like smoking, low vitamin D, or family history), ask your doctor. It’s a simple, painless test.
Can children use steroid inhalers safely?
Yes. Studies show that children on standard doses (under 400 mcg/day of beclomethasone equivalent) grow normally. A small, temporary slowing in growth (about 0.7 cm per year) has been seen, but final adult height isn’t affected. High doses (over 800 mcg/day) should be avoided in children unless absolutely necessary.
What should I do if I think I’m having systemic side effects?
Don’t panic, but don’t ignore it. If you’re unusually tired, bruising easily, losing muscle mass, or feeling dizzy when standing, ask for a salivary cortisol test. It’s non-invasive and can tell you if your adrenal glands are being suppressed. Your doctor can then adjust your dose or switch you to a safer inhaler.
All Comments
winnipeg whitegloves March 22, 2026
Man, I wish I’d known this stuff 10 years ago. I was on fluticasone like it was candy - two puffs, no spacer, no rinse. Hoarse voice? Yeah, I thought I was just singing too loud. Thrush? Thought it was allergies. Then my doc switched me to ciclesonide and slapped a spacer in my hand. Changed everything. No more mouth yeast, no more whispering like a ghost. I’m at 160 mcg now and feel like a new person. Seriously, if you’re on high-dose and not using a spacer - stop reading this and go buy one. It’s like $8 at Walmart.
Also, rinse and spit. Not swallow. I used to swallow like it was medicine. That’s how you get systemic crap. Spit. Like a damn dragon.
And yeah, budesonide over fluticasone? 100%. My pulmonologist said it’s like swapping a flamethrower for a hair dryer. Same heat, less burn.
Marissa Staples March 22, 2026
It’s wild how we treat asthma like it’s a moral failure - like if you’re using steroids, you’re somehow ‘failing’ at being healthy. But breathing is the most basic human function. If you need a tool to do it, that’s not weakness - that’s wisdom. I used to feel guilty about my inhaler. Now I treat it like my coffee maker: essential, non-negotiable, and I clean it after every use. Rinsing? That’s my version of brushing my teeth. Small habits, big difference.
Also, the part about adrenal suppression? I didn’t even know that was a thing. I thought side effects meant ‘dry mouth’ or ‘weight gain.’ Turns out, your body’s own cortisol production can shut down. That’s terrifying. And also… kind of beautiful? That medicine can be this precise. Like a scalpel, not a sledgehammer.
Rachele Tycksen March 23, 2026
so like i was on fluticasone for like 5 years and never used a spacer because i thought it was dumb? turns out i was just spraying it into my throat and eating half the dose? wow. also i forgot to rinse and now my tongue is weird. thanks for the info. also i have no idea what my dose is. i just grab the blue one. oops.
Pat Fur March 25, 2026
My mom’s been on ICS since I was a kid. She’s 72 now. Last year, she started bruising like a peach. We thought it was aging - until I read this. We switched her to budesonide, got her a spacer, and started rinsing. Three months later, her skin stopped turning purple. She’s got more color now than she’s had in years.
And yeah - dose matters. She was on 1000 mcg. We cut it to 400. Still control. No flare-ups. No side effects. It’s not about ‘more is better.’ It’s about ‘enough is enough.’
Also, smart inhalers? Yes. Mine got one for her. It beeps if she forgets to rinse. It’s weird. But it works. She hates it. But she uses it. That’s what matters.
Anil Arekar March 26, 2026
As a healthcare professional with over two decades of clinical experience, I must commend the precision and evidence-based clarity of this post. The distinction between local and systemic side effects is not merely academic - it is foundational to patient safety.
Furthermore, the emphasis on technique, spacer utilization, and dose titration aligns with global guidelines from GINA and the American Thoracic Society. I routinely counsel patients on the pharmacokinetic differences between corticosteroids - particularly the 10-fold variation in systemic absorption between ciclesonide and fluticasone.
It is imperative that primary care providers receive continuing education on these nuances. Too often, asthma management is reduced to a prescription without a protocol. This post serves as a vital corrective.
Elaine Parra March 26, 2026
Look, I don’t care how ‘safe’ you say this is. Steroids are steroids. You think your lungs are special? You think your body won’t break down? I’ve seen patients go from ‘mild asthma’ to full adrenal crisis because some doctor said ‘it’s just an inhaler.’
And don’t get me started on ‘switching inhalers.’ You think your doctor knows what they’re doing? Half of them still think fluticasone is the gold standard. I’ve been on budesonide since 2019. I’m 32. I have zero side effects. My lungs are fine. My bones? Still strong. My skin? Not a bruise in two years.
So if you’re still using fluticasone? You’re playing Russian roulette. And if you’re not rinsing? You’re basically giving yourself a yeast infection on purpose. Wake up.
Natasha Rodríguez Lara March 28, 2026
My dad’s from India and he used to say, ‘If you’re breathing, you’re lucky.’ He had asthma and refused inhalers for years. Said they were ‘Western poison.’ Then he got pneumonia, spent three weeks in the hospital, and came out with a spacer and a new attitude.
He still doesn’t like the word ‘corticosteroid.’ Calls it ‘the quiet medicine.’ I think that’s beautiful. It doesn’t scream. It doesn’t burn. It just… helps. Like a quiet friend who shows up every day.
I started using a spacer last month. I didn’t think I needed it. Now I feel like I’ve been breathing through a straw for 15 years. It’s not magic. It’s just… better.
Caroline Bonner March 29, 2026
Okay, so I just finished reading this entire thing - twice - because I’m obsessed with asthma management (I’m a respiratory therapist, but also just a weirdo who reads medical journals for fun). And I’m so proud of how thorough this is. I mean, the fact that they mentioned eosinophil counts as a biomarker for dose reduction? That’s not even in most primary care guidelines yet!
And the part about ciclesonide having less than 3% systemic absorption? I printed that out and taped it to my fridge. My patient, Mrs. Delaney, was on 1000 mcg of fluticasone - she had bruising, fatigue, and a weird moon face. We switched her to 320 mcg ciclesonide, added a spacer, and she’s been off prednisone for 8 months. No flare-ups. No side effects. She cried when she saw her cortisol levels - they were normal. Normal! After 7 years!
Also, the smart inhaler data? 92% of people think they’re using it right? I’ve seen it. I’ve watched patients inhale like they’re trying to suck a milkshake through a straw. It’s heartbreaking. And so easy to fix. One demo. One spacer. One rinse. That’s it. Why isn’t this mandatory in every asthma clinic? Why isn’t it on Medicare? Why isn’t it taught in high school health class?
And the part about children? I had a 9-year-old patient last month whose growth chart had been flat for a year. We dropped her dose from 800 mcg to 200 mcg. She grew 1.5 cm in six months. Just like that. It’s not about ‘protecting’ kids from steroids - it’s about protecting them from over-treatment.
I’m going to send this to every single patient I have. I’m going to make a handout. I’m going to start a ‘Rinse & Spit’ campaign. Because this isn’t just information - it’s liberation. And it’s free. And it’s right in front of us. We just have to stop being lazy.
Also, I just bought a new spacer. And I’m rinsing now. Because I’m a hypocrite too. And I’m fixing it.