When you're trying to get pregnant, it's easy to focus on ovulation trackers, sperm health, or timing intercourse. But one of the most overlooked factors is your TSH level - a simple blood test that can make a huge difference in whether you conceive and stay pregnant. If your thyroid isn't working right, it can quietly sabotage your chances, even if you feel perfectly fine.
Why TSH Matters Before Pregnancy
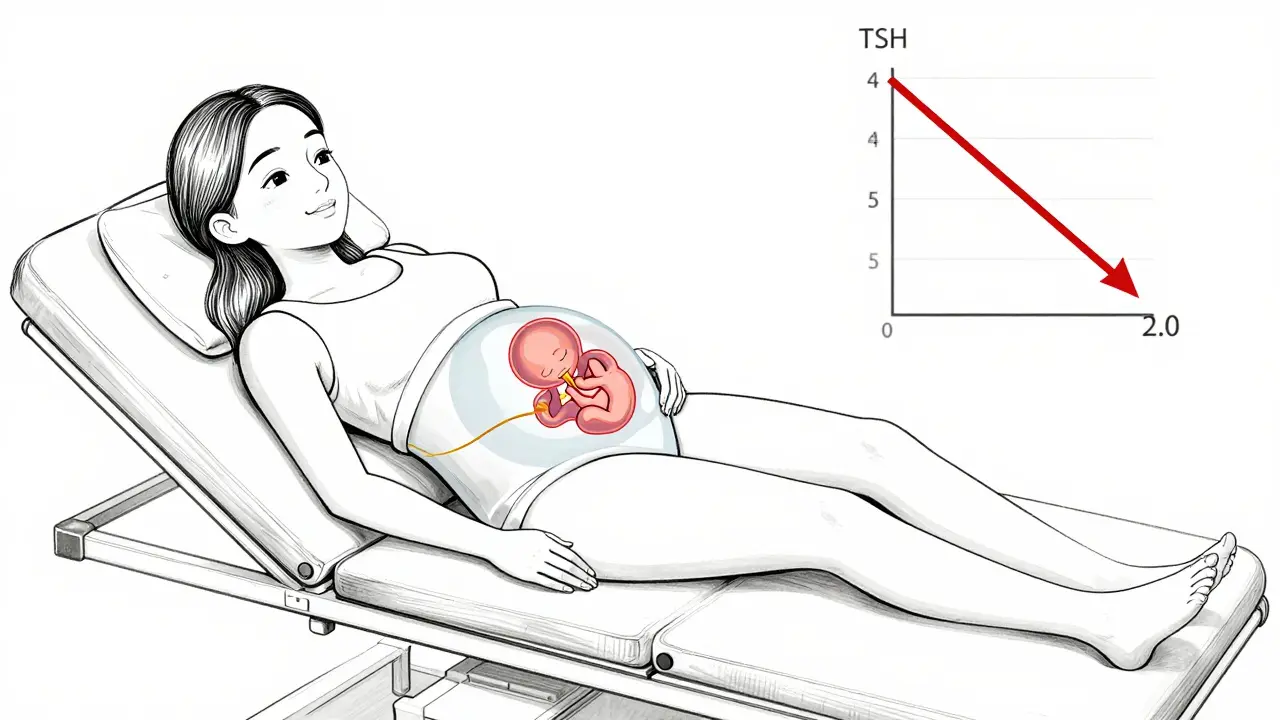
Your thyroid gland makes hormones that control your metabolism, energy, and - critically - your reproductive system. TSH, or thyroid-stimulating hormone, is the signal your brain sends to your thyroid to produce more hormone. If TSH is too high, it means your thyroid isn't making enough. If it's too low, it might be overworking. For someone not trying to get pregnant, a TSH level up to 4.5 mIU/L might be considered normal. But for women planning pregnancy, that range is too wide.
Research shows that even mild thyroid dysfunction can affect ovulation, egg quality, and early embryo development. A 2018 study of over 7,000 women found that nearly twice as many women with unexplained infertility had TSH levels of 2.5 mIU/L or higher compared to those who conceived easily. Another large study of 180,000 women showed that those with TSH levels above 2.5 mIU/L had a 15% higher risk of miscarriage. These aren't rare outliers. They're patterns.
The 2.5 mIU/L Target: What the Experts Say
The American Thyroid Association (ATA) has been clear since 2017: if you have hypothyroidism and are trying to conceive, your TSH should be kept below 2.5 mIU/L. This isn't arbitrary. It's based on how thyroid hormone supports early pregnancy. Before the baby's own thyroid kicks in (around week 10-12), it relies entirely on the mother's supply. If your TSH is above 2.5, your thyroid may not be producing enough hormone to support that critical window.
Organizations like the Endocrine Society and the American Association of Family Physicians agree. Dr. Alex Stagnaro-Green, who led the ATA's guidelines, calls optimizing TSH before conception "one of the most effective preventive interventions we have." It's not just about getting pregnant - it's about staying pregnant.
But here's where things get messy. Some studies, like one from Karakis et al. in 2017, found no difference in pregnancy or live birth rates between women with TSH levels of 2.5-4.5 mIU/L and those below 2.5. These women were undergoing IVF or IUI, and their thyroid antibodies weren't checked. That’s a big blind spot. Because if you have thyroid antibodies - even with normal TSH - your risk of miscarriage goes up.
Thyroid Antibodies: The Hidden Risk
Many women with normal TSH still struggle to conceive or lose pregnancies early. Why? Because they have Hashimoto’s thyroiditis - an autoimmune condition where the body attacks the thyroid. This affects 10-15% of infertile women, compared to just 5-8% in the general population.
The American Society for Reproductive Medicine (ASRM) says women with thyroid antibodies but normal TSH still have a 1-fold increased risk of miscarriage. That means even if your TSH is 2.0, you might need treatment. Studies show that giving these women low-dose levothyroxine reduces miscarriage rates by 45% and increases live birth rates by 36%.
So if you're trying to conceive and have any history of thyroid issues, fatigue, hair loss, or unexplained weight gain - get tested for thyroid antibodies (TPOAb). It’s cheap, simple, and changes your entire plan.
What If You Already Have Hypothyroidism?
If you're already on levothyroxine for hypothyroidism and now want to get pregnant, your dose likely needs to go up - and fast. Most women need a 25-50% increase in their dose as soon as they start trying. Why? Because pregnancy increases the body’s demand for thyroid hormone by up to 50%.
But here’s the problem: a 2019 study found only 37% of women with hypothyroidism got their dose adjusted in time. Many didn’t know they needed to, and their doctors didn’t bring it up. That’s why you can’t assume your current dose is enough. You need to check your TSH before you stop using birth control - not after you miss your period.
For women with Hashimoto’s, the target gets even tighter. Some experts now recommend keeping TSH between 1.25 and 1.75 mIU/L before conception. Why? Because your thyroid is already damaged, and pregnancy will push it further. You need to start with a buffer.
How to Get Your TSH Right
Here’s what to do, step by step:
- Get your TSH and TPOAb tested before you start trying. Don’t wait until you’ve been trying for months.
- If your TSH is above 2.5 mIU/L, talk to your doctor about starting or adjusting levothyroxine. Avoid desiccated thyroid (like Armour thyroid) - it’s not stable enough for pregnancy.
- If you have thyroid antibodies, even with normal TSH, ask if a low-dose levothyroxine (25-50 mcg) might help.
- Retest TSH every 4-6 weeks until you’re below 2.5 mIU/L. It takes about 6 weeks for a dose change to fully affect your levels.
- Once pregnant, increase your dose immediately and retest every 4 weeks through the first trimester. Many women need a 30-50% increase by week 8.
Take your levothyroxine on an empty stomach with water, and wait at least 30 minutes before eating or taking calcium, iron, or antacids. These can block absorption. Many women don’t know this - and end up with under-treated thyroid levels.

What About TSH Below 2.5? Is Lower Better?
Some women worry that if 2.5 is the target, maybe 1.0 is even better. Not necessarily. Going too low can cause symptoms of hyperthyroidism - rapid heartbeat, anxiety, weight loss - and may even harm the pregnancy. The goal isn’t to chase the lowest number. It’s to hit the sweet spot: just enough to support early development without overstimulating your system.
The European Thyroid Association’s 2023 guidelines suggest even tighter targets in early pregnancy: below 1.8 mIU/L in the first 4 weeks, then 2.2 by week 8. But these are still being studied. For now, staying below 2.5 before conception is the safest, most evidence-backed approach.
The Cost of Ignoring It
Levothyroxine costs about $4-$10 a month. A single miscarriage, including medical care and lost work time, can cost over $7,200. A preterm birth? That’s tens of thousands more. One economic analysis found that screening and treating thyroid dysfunction before pregnancy saves $1,850-$2,400 per pregnancy.
And that’s not even counting the emotional toll. Imagine going through months of trying, only to lose a pregnancy because a simple blood test was never done. You don’t need to be diagnosed with full-blown hypothyroidism to benefit. Even borderline levels matter.
What’s Next? New Research on the Horizon
The ATA is currently reviewing updated guidelines, expected in 2026. A major NIH-funded trial (NCT03856002) is testing whether personalized TSH targets - based on your thyroid reserve and antibody status - lead to better outcomes than the one-size-fits-all 2.5 mIU/L target. Early results suggest women with low thyroid reserve might need TSH below 1.5, while others might do fine closer to 2.5.
But you don’t need to wait for new guidelines. The evidence we have now is strong enough to act. If you’re trying to conceive and haven’t checked your thyroid, do it now. It’s one of the easiest, cheapest, and most effective things you can do to improve your chances.
Can I get pregnant if my TSH is above 2.5?
Yes, you can - but your chances of miscarriage and infertility increase. Studies show women with TSH above 2.5 mIU/L have a higher risk of not conceiving or losing the pregnancy early. It doesn’t mean you can’t get pregnant, but it does mean you’re fighting an uphill battle. Optimizing your TSH before conception improves your odds significantly.
Do I need to get tested if I don’t have symptoms?
Absolutely. Many women with thyroid dysfunction feel perfectly fine. Fatigue, weight gain, and irregular periods are often blamed on stress or aging - but they can be signs of an underactive thyroid. Since thyroid issues are so common in women trying to conceive (15-20% have abnormal TSH), screening is recommended for everyone in this group, not just those with symptoms.
Is levothyroxine safe during preconception and pregnancy?
Yes, and it’s the standard treatment. Levothyroxine is a synthetic form of the thyroid hormone your body naturally makes. It’s safe for both mother and baby and is essential for fetal brain development. Desiccated thyroid (like Armour) is not recommended because it contains T3, which can cause unstable hormone levels during pregnancy.
How often should I test my TSH when trying to conceive?
Test every 4-6 weeks while adjusting your dose. Once your TSH is stable below 2.5 mIU/L, you can space tests out to every 8-12 weeks. But if you start a new medication, change your dose, or gain/lose weight, test again. Your thyroid needs don’t stay the same - especially when you’re trying to get pregnant.
Should I get tested if I’ve had a miscarriage before?
Yes. Recurrent miscarriage is one of the clearest red flags for thyroid dysfunction. Even if your TSH was normal before, it’s worth retesting. Thyroid antibodies can develop over time, and many women only discover their issue after losing a pregnancy. Testing is simple, non-invasive, and could prevent future losses.
All Comments
Helen Brown March 2, 2026
The government and pharmaceutical companies are hiding the truth about thyroid meds. They want you dependent on levothyroxine so they can sell you more pills. Natural remedies like selenium and iodine work better. I’ve seen it myself. They don’t want you to know this. Your doctor won’t tell you. But now you do.
John Cyrus March 2, 2026
If your TSH is above 2.5 and you're trying to get pregnant you're already behind the curve. Stop wasting time. Get tested. Take the pill. Case closed. No need to overthink it. I've seen too many women delay this and regret it later. It's not rocket science.
Sharon Lammas March 3, 2026
It’s fascinating how we’ve turned something as natural as fertility into a series of numbers to optimize. TSH 2.5 feels like a boundary we built to feel in control. But what if the body knows more than the lab? What if some women thrive with higher levels and just need rest, not medication? I wonder if we’re missing the deeper rhythm beneath the numbers.
marjorie arsenault March 3, 2026
If you're trying to conceive and haven't checked your thyroid, do it now. It's simple. It's cheap. It could change everything. I’ve helped so many women through this. One client went from three miscarriages to a healthy baby after starting low-dose levothyroxine. She didn’t even feel sick. That’s the scary part. You don’t need to feel bad to be out of balance. Get tested. Talk to your doctor. Don’t wait.
Deborah Dennis March 5, 2026
I'm sorry, but this article is way too alarmist. You're scaring women into taking medication they don't need. TSH 2.5? That's not a cliff. It's a gentle slope. And you're ignoring the fact that many women with high TSH still conceive just fine. Also, levothyroxine isn't harmless-it can cause heart palpitations, anxiety, bone loss. You're not giving the full picture. This is irresponsible.
Shivam Pawa March 6, 2026
Thyroid dysfunction is underdiagnosed in South Asia too. Many women present with fatigue, hair fall, irregular cycles. TSH >2.5 is common. Levothyroxine is safe. But we need better screening access. In rural clinics, even TSH tests are rare. Policy change > individual action. We need national guidelines, not just blog posts.
Diane Croft March 7, 2026
You’ve got this. One blood test. One conversation with your doctor. One small step. That’s all it takes to give your future baby the best start. I believe in you. You’re not alone in this journey. Keep going. You’re doing better than you think.
Donna Zurick March 9, 2026
I had a miscarriage at 8 weeks. My TSH was 3.8. No symptoms. No idea. After I started levothyroxine, got pregnant again in 3 months. Now I have a 2-year-old. This saved me. If you're trying, get tested. It’s not scary. It’s just smart.